What Is Living Intelligence in Health Tech?
Living intelligence in health tech refers to intelligent systems that continuously interact with biological signals and adapt their behavior over time, transforming healthcare from a reactive, episodic discipline into a continuous, predictive one.
Unlike traditional AI systems trained on static datasets, living intelligence systems:
- Continuously ingest sensor and biological data
- Learn from real-time physiological feedback
- Adjust clinical decisions dynamically
- Operate reliably in uncertain, real-world environments
In practical terms, this means AI systems that co-evolve with the patient’s own physiological state, not a tool that runs once and stops, but one that keeps listening, learning, and responding.
Key insight : Living intelligence is not a product category. It is an architectural paradigm, a way of designing health systems that behave more like organisms than software.
Why Living Intelligence Matters: The Problem It Solve
Traditional healthcare systems are structurally limited in three ways:
1. Reactive, not predictive. Care is triggered by symptoms, by the time a problem is detectable, damage has already occurred.
2. Episodic, not continuous. A patient’s health data exists mostly during clinical visits, leaving large gaps in understanding.
3. Population-based, not personalized. Treatment protocols are designed for average patients, not individual biology.
Living intelligence directly addresses all three. It enables health systems to shift from treating disease to preventing it, and from managing populations to serving individuals.
The Three Core Layers of Living Intelligence
Living intelligence in healthcare relies on three tightly integrated layers working in continuous feedback.
1. AI and Machine Learning
AI models process complex, high-frequency biomedical data at scales no human clinician can match alone. Core techniques include:
- Deep learning for medical signal analysis (ECG, EEG, imaging)
- Time-series models for tracking physiological trends over time
- Reinforcement learning for adaptive treatment strategies
- Probabilistic models for handling uncertainty in clinical data
These models do not replace clinicians. They extend what clinicians can perceive and act on, flagging patterns, surfacing anomalies, and supporting faster, more informed decisions.
Discover : Beginner roadmap to deep learning 2026 : Tools, courses & Algeria | Around Data Science
2. Biotechnology and Biological Interfaces
Biotechnology gives AI systems access to biological signals at multiple scales. This includes:
- Genomic and proteomic data
- Biomarkers extracted from blood or tissue
- Neural and muscular electrical signals
- Metabolic and hormonal indicators
This layer is what grounds living intelligence in biological reality rather than abstract data. Without it, AI in healthcare is modeling approximations.
3. Sensor and Embedded Systems
Sensors are the nervous system of living intelligence. Without continuous data acquisition, the entire system collapses into batch processing. Key sensor types include:
- Wearable biosensors (heart rate, glucose, oxygen, temperature)
- Implantable medical devices (neurostimulators, cardiac monitors)
- Smart imaging systems (AI-assisted radiology and pathology)
- Environmental and behavioral sensors (ambient data, activity tracking)
These devices enable the continuous, real-time data streams that make adaptive health intelligence possible.
Read more : Case Studies | Around Data Science
How Living Intelligence Works: The Adaptive Loop
Living intelligence systems operate as closed adaptive loops, a cycle that never stops running.
Sensing → Data Fusion → AI Interpretation → Decision / Action → Feedback & Learning → SensingStep 1 — Sensing: Continuous acquisition of biological and behavioral signals from wearables, implants, and smart devices.
Step 2 — Data fusion: Integration of multimodal data streams, combining cardiac signals, metabolic readings, genomic context, and behavioral patterns.
Step 3 — AI-driven interpretation: Pattern recognition, anomaly detection, and risk scoring in real time.
Step 4 — Decision support or action: Alerts sent to clinicians, adaptive device adjustments, or automated interventions.
Step 5 — Feedback and learning: The system updates its models based on outcomes, becoming more accurate over time.
This loop never stops. That is what makes it “living.”
Real-World Applications in Health Tech
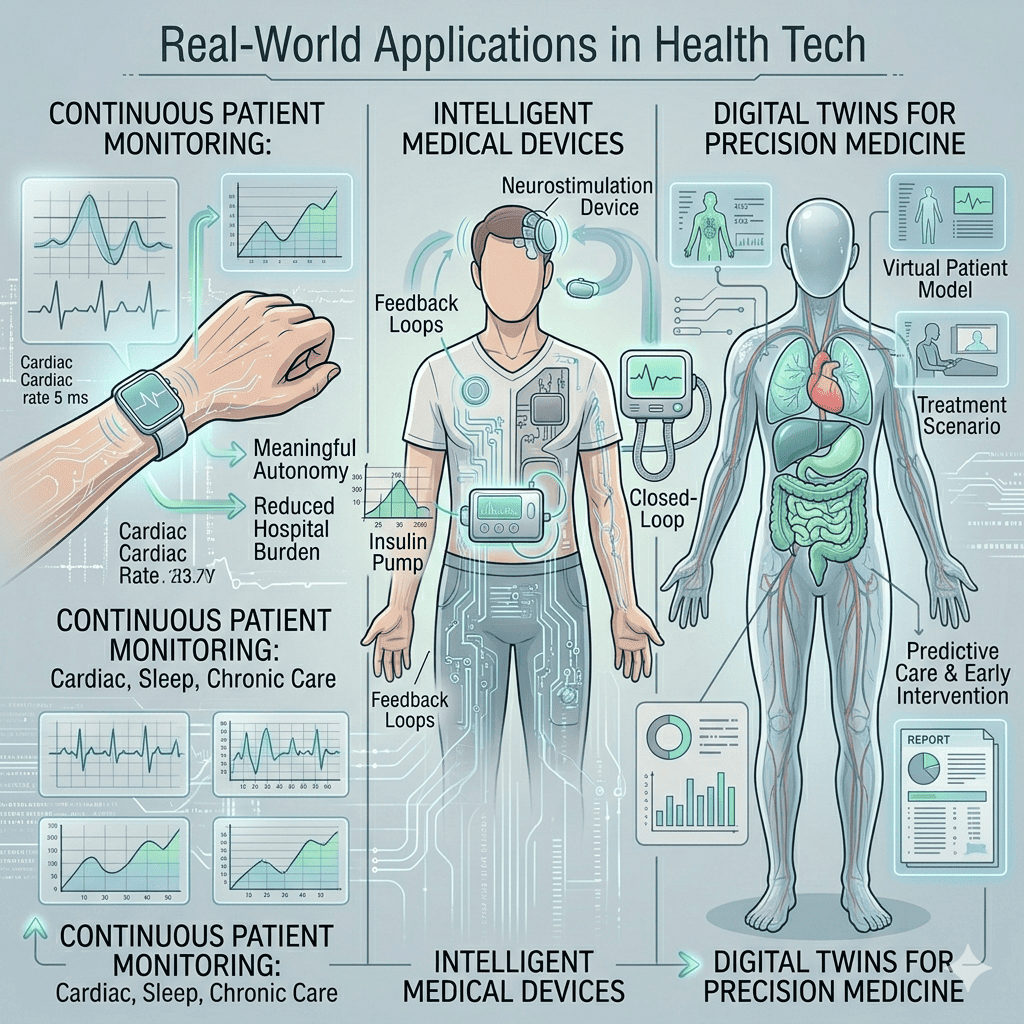
Continuous Patient Monitoring
AI-powered wearables now enable long-term health monitoring outside clinical settings. Key applications include:
- Cardiac rhythm monitoring and arrhythmia detection
- Sleep disorder identification and management
- Chronic disease tracking (diabetes, COPD, hypertension)
This reduces hospital burden, extends care reach, and gives patients meaningful autonomy over their own health data.
Intelligent Medical Devices
A growing category of devices now behaves like cyber-biological systems, sensing, deciding, and acting within a single unit:
- Smart insulin pumps with adaptive, real-time dosing
- Neurostimulation devices that respond to neural feedback
- Closed-loop ventilators that adjust to patient breathing patterns
These are no longer passive tools. They are responsive, learning systems embedded in the body.
Digital Twins for Precision Medicine
Digital twins replicate patient physiology in a virtual environment. This allows clinicians to:
- Simulate treatment scenarios before applying them
- Run risk-free experiments on virtual patient models
- Generate personalized prognosis estimates
Digital twin technology is gaining serious traction in oncology, cardiology, and rare disease management, anywhere the cost of trial-and-error is too high.
Predictive Care and Early Intervention
This is where living intelligence delivers its most dramatic clinical value. Examples include:
- Predicting cardiac events from subtle ECG trend shifts hours before onset
- Detecting glucose anomalies before dangerous thresholds are crossed
- Anticipating neurological episodes through early neural pattern changes
Prediction replaces reaction. That is a structural improvement in patient outcomes.
Learn more about : Prediction Metrics in Machine Learning and Time Series Forecasting | Around Data Science
Benefits vs. Challenges: An Honest Assessment
Key Advantages
| Benefit | Clinical Impact |
|---|---|
| Continuous monitoring | Earlier detection, earlier intervention |
| Adaptive intelligence | Genuinely personalized care |
| Data-driven insights | Better-informed clinical decisions |
| Automation | Reduced clinician cognitive load |
Key Challenges
Living intelligence introduces real complexity that cannot be glossed over:
Data privacy and security: Biological data is among the most sensitive data that exists. Living intelligence systems aggregate it continuously. Governance frameworks must be robust, not performative.
Model interpretability: Black-box AI in clinical settings is a liability. Clinicians need to understand why a model flags a risk, not just that it did.
Regulatory approval: Moving from prototype to approved clinical tool remains slow, expensive, and jurisdiction-dependent. This is a real bottleneck for the field.
Ethical use of biological data: Who owns the data? Who benefits from the models trained on it? These questions are not yet resolved at scale.
Living intelligence must remain human-centered and transparent, or it will erode the trust it depends on.
5 Practical Tips for Building Living Intelligence Systems
- Start with high-quality, calibrated sensors. Garbage in, garbage out, unreliable sensing corrupts every downstream layer.
- Prioritize explainable AI models. If a clinician cannot interrogate a decision, they cannot trust it, and they shouldn’t have to.
- Design for interoperability from day one. Health data lives in silos. Systems that cannot communicate cannot learn.
- Integrate clinicians early in the design process. The best sensor array in the world fails if it generates alerts no one can act on.
- Build privacy by design, not by compliance. Consent, data minimization, and anonymization should be architecture — not afterthoughts bolted on at the end.
Bonus: Build an online platform around your AI system
If you’re planning to create a web interface, showcase your AI projects, or even sell hardware or AI-based services, you’ll need a reliable store builder.
🔥 If you’re looking to build a high-performing online store while keeping things simple, check out Ayor.ai.
It’s an AI-powered e-commerce platform designed to help you launch, optimize, and scale your store in Algeria or globally.
Frequently Asked Questions
1. What makes living intelligence different from traditional AI in healthcare?
Traditional healthcare AI analyzes historical datasets and produces static outputs. Living intelligence continuously ingests real-time biological signals and adapts its behavior over time, closing the loop between sensing, decision-making, and learning.
2. Is living intelligence safe for patients?
When properly validated, regulated, and transparently designed, yes. The critical safeguards are clinical validation, regulatory approval, explainability, and strong data governance.
3. Does living intelligence replace doctors?
No. It extends what doctors can perceive, process, and act on. The clinical judgment, ethical accountability, and patient relationship remain human.
4. Where is living intelligence already in use today?
The most mature applications are in wearable cardiac monitors, continuous glucose monitoring, smart insulin delivery, and AI-assisted diagnostic imaging. Digital twins are emerging rapidly in precision medicine.
5. What expertise is needed to build these systems?
Living intelligence sits at the intersection of AI engineering, biomedical engineering, embedded systems design, clinical science, and applied ethics. Cross-disciplinary teams are not optional, they are the prerequisite.
6. Will the cost of deployment fall over time?
Yes. Sensor hardware costs are declining sharply. AI model training costs are dropping. The primary cost driver shifting forward is regulatory compliance and clinical validation, not technology.
The Future of Living Intelligence in Health Tech
Living intelligence is not an incremental improvement to existing health technology. It is a structural shift in how health systems perceive, understand, and respond to the human body.
The future of healthcare is not software that runs when prompted. It is systems that sense continuously, learn persistently, and act adaptively, always in service of the patient, always within a framework of human oversight.
The trajectory is clear. The question for practitioners, developers, and policymakers is not whether living intelligence will reshape health tech. It is whether the systems being built today are designed with the rigor, transparency, and ethics that this transformation demands.
👉 Join the Around Data Science community on Discord, subscribe to our newsletter, and follow us on LinkedIn for more free resources and career tips.





0 Comments